Disparities in Health and Health Care: 5 Key Questions and Answers

Table of Contents
Introduction
The COVID-19 pandemic and nationwide racial justice movement over the past several years have heightened the focus on health disparities and their underlying causes and contributed to the increased prioritization of health equity. These disparities are not new and reflect longstanding structural and systemic inequities rooted in racism and discrimination. Although growing efforts have focused recently on addressing disparities, the ending of some policies implemented during the COVID-19 pandemic, including continuous enrollment for Medicaid and the Children’s Health Insurance Program (CHIP), may reverse progress and widen disparities. Addressing health disparities is not only important from an equity standpoint, but also for improving the nation’s overall health and economic prosperity. This brief provides an introduction to what health and health care disparities are, why it is important to address disparities, what the status of disparities is today, recent federal actions to address disparities, and key issues related to addressing disparities looking ahead.
What are health and health care disparities?
Health and health care disparities refer to differences in health and health care between groups that stem from broader inequities. There are multiple definitions of health disparities. Healthy People 2030 defines a health disparity, as “a particular type of health difference that is linked with social, economic, and/or environmental disadvantage,” and that adversely affects groups of people who have systematically experienced greater obstacles to health. The Centers for Disease Control and Prevention (CDC) defines health disparities as, “preventable differences in the burden, disease, injury, violence, or in opportunities to achieve optimal health experienced by socially disadvantaged racial, ethnic, and other population groups and communities.” A health care disparity typically refers to differences between groups in health insurance coverage, affordability, access to and use of care, and quality of care. The terms “health inequality” and “inequity” are also sometimes used to describe unjust differences. Racism, which the CDC defines as the structures, policies, practices, and norms that assign value and determine opportunities based on the way people look or the color of their skin, results in conditions that unfairly advantage some and disadvantage others, placing people of color at greater risk for poor health outcomes.
Health equity generally refers to individuals achieving their highest level of health through the elimination of disparities in health and health care. Healthy People 2030 defines health equity as the attainment of the highest level of health for all people and notes that it requires valuing everyone equally with focused and ongoing societal efforts to address avoidable inequalities, historical and contemporary injustices, and health and health care disparities. The CDC describes health equity as when everyone has the opportunity to be as healthy as possible.
A broad array of factors within and beyond the health care system drive disparities in health and health care (Figure 1). Though health care is essential to health, research shows that health outcomes are driven by multiple factors, including underlying genetics, health behaviors, social and environmental factors, and access to health care. While there is currently no consensus in the research on the magnitude of the relative contributions of each of these factors to health, studies suggest that health behaviors and social and economic factors, often referred to as social determinants of health, are the primary drivers of health outcomes and that social and economic factors shape individuals’ health behaviors. Moreover, racism negatively affects mental and physical health both directly and by creating inequities across the social determinants of health.
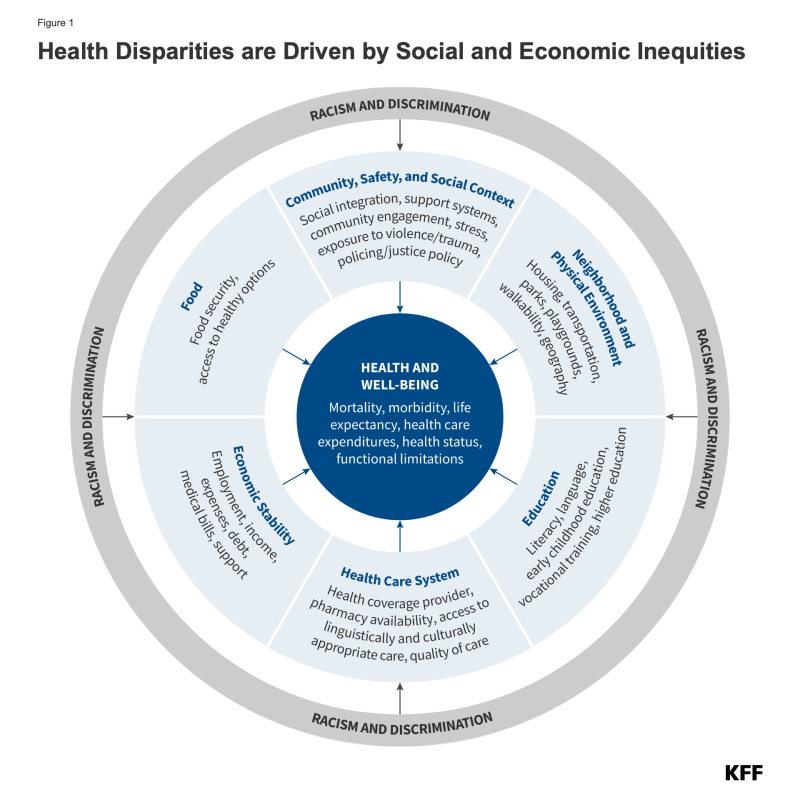
Figure 1: Health Disparities are Driven by Social and Economic Inequities
Health and health care disparities are often viewed through the lens of race and ethnicity, but they occur across a broad range of dimensions. For example, disparities occur across socioeconomic status, age, geography, language, gender, disability status, citizenship status, and sexual identity and orientation. Research also suggests that disparities occur across the life course, from birth, through mid-life, and among older adults. Federal efforts to reduce disparities focus on designated priority populations, including, “members of underserved communities: Black, Latino, and Indigenous and Native American persons, Asian Americans and Pacific Islanders and other persons of color; members of religious minorities; lesbian, gay, bisexual, transgender, and queer (LGBT+) persons; persons with disabilities; persons who live in rural areas; and persons otherwise adversely affected by persistent poverty or inequality.” These groups are not mutually exclusive and often intersect in meaningful ways. Disparities also occur within subgroups of populations. For example, there are differences among Hispanic people in health and health care based on length of time in the country, primary language, and immigration status. Data often also mask underlying disparities among subgroups within the Asian population.
Why is it important to address disparities?
Addressing disparities in health and health care is important not only from an equity standpoint but also for improving the nation’s overall health and economic prosperity. People of color and other underserved groups experience higher rates of illness and death across a wide range of health conditions, limiting the overall health of the nation. Research further finds that health disparities are costly, resulting in excess medical care costs and lost productivity as well as additional economic losses due to premature deaths each year.
It is increasingly important to address health disparities as the population becomes more diverse and income inequality continues to grow. It is projected that people of color will account for over half (52%) of the population in 2050, with the largest growth occurring among people who identify as Asian or Hispanic (Figure 2). Over time, the population has become increasingly racially diverse, reflecting shifting immigration patterns, a growing multiracial population, as well as adjustments to how the federal Census Bureau measures race and ethnicity. Over time, income inequality within the U.S. has also widened. As of 2021, the richest 20% of households accounted for over half of the aggregate household income and had an income of $149,132 or higher compared to the bottom 20% of households who accounted for less than 3% of the aggregate household income and had incomes of $28,007 or less. The top 5 percent of households in the income distribution had incomes of $286,305 or more. Research suggests that the disparate negative effects of the COVID-19 pandemic on lower-paid occupations may have lingering effects that contribute to further widening income inequality over the long term.
What is the status of disparities today?
Disparities in health and health care are persistent and prevalent. Major recognition of health disparities began more than three decades ago with the Report of the Secretary’s Task Force on Black and Minority Health (Heckler Report) in 1985, which documented persistent health disparities that accounted for 60,000 excess deaths each year and synthesized ways to advance health equity. The Heckler Report led to the creation of the U.S. Department of Health and Human Services Office of Minority Health and influenced federal recognition of and investment in many aspects of health equity. In 2003, the Institute of Medicine’s Committee on Understanding and Eliminating Racial and Ethnic Disparities in Health Care released the report, Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care, which identified systemic racism as a major cause of health disparities in the United States. Despite the recognition and documentation of disparities for decades and overall improvements in population health over time, many disparities have persisted, and, in some cases, widened over time.
Despite large gains in coverage since implementation of the Patient Protection and Affordable Care Act (ACA) in 2014, people of color and other marginalized and underserved groups remain more likely to be uninsured. Racial disparities in coverage persisted as of 2021, with higher uninsured rates for nonelderly American Indian or Alaska Native (AIAN), Hispanic, Black, and Native Hawaiian or Pacific Islander (NHOPI) people compared to their White counterparts (Figure 3). Other groups also remained at increased risk of being uninsured, including immigrants and people in lower-income families. Many people who are uninsured are eligible for coverage through Medicaid, CHIP, or the ACA Marketplaces but face barriers to enrollment including confusion about eligibility policies, difficulty navigating enrollment processes, and language and literacy problems. Some immigrant families also have immigration-related fears about enrolling themselves or their children in Medicaid or CHIP even if they are eligible. Others remain ineligible because their state did not expand Medicaid, due to their immigration status, or because they have access to an affordable Marketplace plan or offer of employer coverage.
Beyond coverage, people of color and other marginalized and underserved groups continue to experience many disparities in accessing and receiving care. For example, people in rural areas face barriers to accessing care due to low density of providers and longer travel times to care, as well as more limited access to health coverage. There also are inequities in experiences receiving health care across groups. For example, the KFF/The Undefeated 2020 Survey on Race and Health, found that one in five Black adults and one in five Hispanic adults report being treated unfairly treatment due to their race or ethnicity while getting health care for themselves or a family member in the past year. Nearly one-quarter (24%) of Hispanic adults and over one in three (34%) potentially undocumented Hispanic adults reported that it was very or somewhat difficult to find a doctor who explains this in a way that is easy to understand in a 2021 KFF survey. Other KFF survey data from 2022 found that nearly one in ten (9%) of nonelderly adult women who visited a health care provider in the past two years said they experienced discrimination because of their age, gender, race, sexual orientation, religion, or some other personal characteristic during a health care visit. KFF data also showed that LGBT+ people were more likely than their non-LGBT+ counterparts to report certain negative experiences while getting health care, including a doctor not believing they were telling the truth, suggesting they are personally to blame for a health problem, assuming something about them without asking, and/or dismissing their concerns. The 2023 KFF/The Washington Post Trans Survey found that trans adults were more likely to report having difficulty finding affordable health care or a provider who treated them with dignity and respect compared to cisgender adults.
People of color and other underserved groups face ongoing disparities in health. For example, at birth, AIAN and Black people had shorter life expectancies compared to White people as of 2021, and AIAN, Hispanic, and Black people experienced larger declines in life expectancy than White people between 2019 and 2021, reflecting the impacts of COVID-19 (Figure 4). Black infants were more than two times as likely to die as White infants and AIAN infants were nearly twice as likely to die as White infants as of 2021. Black and AIAN women also had the highest rates of pregnancy-related mortality across groups. Rates of chronic disease and cancer also vary by race and ethnicity. Although Black people did not have higher cancer incidence rates than White people overall and across most types of cancer, they were more likely to die from cancer in 2019. There are also stark disparities in health by income. Research shows that people living in areas with high concentrations of poverty are at increased risk of poorer health outcomes over the course of their lives. KFF analysis also found that LGBT+ people were more likely to report being in fair or poor health and having an ongoing health condition that requires ongoing monitoring, medical care, or medication compared to non-LGBT+ people despite being a younger population.
The COVID-19 pandemic has taken a disproportionate toll on the health and well-being of people of color and other underserved groups. Cumulative age-adjusted data showed that AIAN and Hispanic people have had a higher risk for COVID-19 infection and AIAN, Hispanic, and Black people have had a higher risk for hospitalization and death due to COVID-19. Beyond these direct health impacts, the pandemic has negatively impacted the mental health, well-being, and social and economic factors that drive health for people of color and other underserved groups, including LGBT+ people. As such, the pandemic may contribute to worsening health disparities going forward.
Concerns about mental health and substance use have increased since the onset of the pandemic, particularly among some groups. According to a 2022 KFF/CNN survey, 90% of the public think there is a mental health crisis in the U.S. today. Over the course of the pandemic, many adults reported symptoms consistent with anxiety and depression. Additionally, drug overdose deaths have sharply increased – largely due to fentanyl – and after a brief period of decline, suicide deaths are once again on the rise. These negative mental health and substance use outcomes have disproportionately affected some populations, particularly communities of color and youth. Drug overdose death rates were highest among AIAN and Black people as of 2021. Alcohol-induced death rates increased substantially during the pandemic, with rates increasing the fastest among people of color and people living in rural areas. From 2019 to 2021, many people of color experienced a larger growth in suicide death rates compared to their White counterparts. Additionally, self-harm and suicidal ideation has increased faster among adolescent females compared to their male peers. Findings from a 2023 KFF/The Washington Post survey found that more trans adults reported struggling with serious mental health issues compared to cisgender adults and were six times as likely as cisgender adults to have engaged in self-harm in the previous year (17% vs. 3%). There are also substantial disparities in mental health, including suicidality, among LGBT+ youth compared to their non-LGBT+ peers.
What are recent federal actions to address disparities?
In the wake of the COVID-19 pandemic, there has been a heightened awareness of and focus on addressing health disparities. The disparate impacts of COVID-19 and coinciding racial reckoning following the police killing of George Floyd contributed to a growing awareness of racial disparities in health and their underlying causes, including racism. Early in his presidency, President Biden issued a series of executive orders focused on advancing health equity, including orders that outlined equity as a priority for the federal government broadly and as part of the pandemic response and recovery efforts. Federal agencies were directed with developing Equity Action Plans that outlined concrete strategies and commitments to addressing systemic barriers across the federal government. In its Health Equity Plan, the Department of Health and Human Services (HHS) outlined a series of new strategies, including addressing increased pregnancy and postpartum morbidity and mortality among Black and AIAN women; addressing barriers that individuals with limited English proficiency face in obtaining information, services, and benefits from HHS programs; leveraging grants to incorporate equity consideration into funding opportunities, implementing equity assessments across its major policies and programs; investing in resources to advance civil rights; and expanding contracting opportunities for small, disadvantaged businesses. The plan builds on earlier efforts that included increasing stakeholder engagement, establishing the Office of Climate Change and Health Equity, and establishing the National Institutes of Health UNITE Initiative to address structural racism and racial inequities in biomedical research. Since the release of its Equity Action Plan, HHS has taken actions to extend postpartum coverage through Medicaid and CHIP; issued rules to strengthen patient protections, including nondiscrimination protections; and issued nondiscrimination guidance to ensure that telehealth services are accessible to people with disabilities and those with limited English proficiency.
The Centers for Medicare and Medicaid Services (CMS) released an updated framework to advance health equity, expand health coverage, and improve health outcomes for people covered by Medicare, Medicaid, CHIP, and the Health Insurance Marketplaces. The framework outlined five priorities including expanding the collecting, reporting, and analysis of standardized data on demographics and social determinants of health; assessing the causes of disparities within CMS programs and addressing inequities in policies and operations; building capacity of health care organizations and the workforce to reduce disparities; advancing language access, health literacy, and the provision of culturally tailored services; and increasing all forms of accessibility to health services and coverage. The Administration has also identified advancing health equity and addressing social determinants of health as key priorities within Medicaid and has encouraged states to propose Section 1115 Medicaid waivers that expand coverage, reduce health disparities, and/or advance “whole-person care.” States have increasingly requested and/or received approval for waivers that aim to advance equity. Further, a growing number of states have approved or pending waivers with provisions related to addressing health-related social needs, such as food and housing, often focused on specific populations with high needs or risks.
The Administration and Congress have taken a range of actions to stabilize and increase access to health coverage amid the pandemic. Early in the pandemic, Congress passed the Families First Coronavirus Response Act (FFCRA), which included a temporary requirement that Medicaid programs keep people continuously enrolled during the COVID-19 Public Health Emergency in exchange for enhanced federal funds. Primarily due to the continuous enrollment provision, Medicaid enrollment has grown substantially compared to before the pandemic, and the uninsured rate has dropped with differences in uninsured rates between people of color and White people narrowing. Coverage gains also likely reflected enhanced ACA Marketplace subsidies made available by the American Rescue Plan Act (ARPA) of 2021 and renewed for another three years in the Inflation Reduction Act of 2022, boosted outreach and enrollment efforts, a Special Enrollment Period for the Marketplaces provided in response to the pandemic, and low Marketplace attrition. Additionally, in 2019, the Biden Administration reversed changes the Trump Administration had previously made to public charge immigration policies that increased reluctance among some immigrant families to enroll in public programs, including health coverage. Most recently, the Consolidated Appropriations Act of 2023 included a requirement for all states to implement 12 months of continuous coverage for children, supporting their coverage stability. However, it also set the end of the broader Medicaid continuous enrollment provision for March 31, 2023, which could lead to coverage losses for millions of people, reversing recent coverage gains.
There have been growing federal efforts to address disparities in maternal health. Over the past few years, the Administration launched several initiatives focused on addressing inequities in maternal health. In April 2021, President Biden issued a proclamation to recognize the importance of addressing the high rates of maternal mortality and morbidity among Black people. At the end of 2021, the White House hosted its inaugural White House Maternal Health Day of Action during which areas of concern in maternal health outcomes were identified and the Administration announced actions aimed at solving the maternal health crisis. In June 2022, the Biden Administration released the Blueprint for Addressing the Maternal Health Crisis. The Blueprint outlines priorities and actions across federal agencies to improve access to coverage and care, expand and enhance data collection and research, grow and diversify the perinatal workforce, strengthen social and economic support, and increase trainings and incentives to support women being active participants in their care before, during and after pregnancy. In July 2022, CMS announced a Maternity Care Action Plan to support the implementation of the Biden-Harris Administration’s Blueprint for Addressing the Maternal Health Crisis. The action plan takes a holistic and coordinated approach across CMS to improve health outcomes and reduce inequities for people during pregnancy, childbirth, and the postpartum period. ARPA included an option, made permanent in the Consolidated Appropriations Act, to allow states to extend Medicaid postpartum coverage from 60 days to 12 months. As of April 2023, the majority of states have taken steps to extend postpartum coverage. The Human Resources and Services Administration also announced $12 million in awards for the Rural Maternal and Obstetrics Management Strategies Program (RMOMS), which is designed to develop models and implement strategies to improve maternal health in rural communities.
The Administration has also taken steps to address health disparities and discrimination experienced among LGBT+ people. On his first day in office, President Biden signed an Executive Order on “Preventing and Combating Discrimination on the Basis of Gender Identity or Sexual Orientation.” Since then, the Administration has taken multiple actions to address discrimination within health care specifically. In May 2021, the Biden Administration announced that the HHS Office for Civil Rights (OCR) would include gender identity and sexual orientation as it interprets and enforces the ACA’s prohibition against sex discrimination (Section 1557), reversing the approach taken by the Trump Administration. Additionally, the Administration has spoken out against state actions aimed at curtailing access to gender affirming care for transgender and gender nonconforming people, particularly policies targeting youth. In January 2023, the Administration released its Federal Evidence Agenda on LGBTQI+ Equity, a “roadmap for federal agencies as they work to create their own data-driven and measurable SOGI Data,” which the Administration views as central to understanding disparities and discrimination facing this community.
What are key issues related to health disparities looking ahead?
The end of the Medicaid continuous enrollment provision may lead to coverage losses and widening disparities. Following the ending of the Medicaid continuous enrollment provision on March 31, 2023, states resumed Medicaid redeterminations. KFF estimates that between 5 and 14 million people could lose Medicaid coverage, including many who newly gained coverage during the pandemic. Other research shows that Hispanic and Black people are likely to be disproportionately impacted by the expiration of the continuous enrollment provision. Moreover, some groups, such as individuals with limited English proficiency and people with disabilities may face increased challenges in completing the Medicaid renewal process increasing their risk of coverage loss even if they remain eligible for coverage. OCR has reminded states of their obligations under federal civil rights laws to take reasonable steps to provide meaningful language access for individuals with limited English proficiency and ensure effective communication with individuals with disabilities to prevent lapses in coverage amid the unwinding of the continuous enrollment provision. CMS issued guidance that provides a roadmap for states to streamline processes and implement strategies to reduce the number of people who lose coverage even though they remain eligible. The extent to which states simplify processes to renew or transition to other coverage and provide outreach and assistance to individuals more likely to face challenges completing renewal processes will impact coverage losses and potential impacts on coverage disparities.
The end of the COVID-19 Public Health Emergency (PHE) and the potential depletion of the federally purchased supply of COVID-19 vaccines, treatments, and tests may curtail access to these supplies for some individuals, particularly those who are uninsured. In response to the COVID-19 pandemic, the federal government spent billions of dollars in emergency funds to purchase COVID-19 vaccines, including boosters, treatments, and tests to provide free of charge to the public. In addition, Congress enacted legislation that included special requirements for their coverage by both public and private insurers, and the Administration issued guidance and regulations to protect patient access and promote equitable distribution. The upcoming end to the PHE on May 11, 2023, as well as the potential depletion of federally purchased supplies in the absence of any additional funding, could result in new or higher cost-sharing and/or reduced access to these products although these impacts may vary by product and the type of health coverage an individual has. People who are uninsured or underinsured face the greatest risk of access challenges, including limited access to free vaccines and no coverage for treatment or tests. Since people of color and people with lower incomes are more likely to be uninsured, they may be at a disproportionate risk of facing barriers to accessing COVID-19 vaccines, tests, and treatments once the PHE ends and the federal supply is depleted.
The overturning of Roe v. Wade may exacerbate the already large racial disparities in maternal and infant health. The decision to overturn the longstanding Constitutional right to abortion and elimination of federal standards on abortion access has resulted in growing variation across states in laws protecting or restricting abortion. These changes may disproportionately impact women of color, as they are more likely to obtain abortions, have more limited access to health care, and face underlying inequities that would make it more difficult to travel out of state for an abortion compared to their White counterparts. Restricted access to abortions may widen the already stark racial disparities in maternal and infant health, as some groups of color are at higher risk of dying from pregnancy-related reasons and during infancy and are more likely to experience birth risks and adverse birth outcomes compared to White people. It may also have negative economic consequences associated with the direct costs of raising children and impacts on educational and employment opportunities. Further, women from underserved communities may be at increased risk for criminalization in a post-Roe environment, as prior to the ruling, there were already cases of women being criminalized for their miscarriages, stillbirths, or infant death, many of whom were low-income or women of color.
Many states have implemented policies banning or limiting access to gender affirming care, especially for youth, as well as other legal actions that threaten access to care for LGBT+ people. Policies aimed at limiting access to gender affirming care may have significant negative implications for the health of trans and nonconforming people, particularly young people, including negative mental health impacts, and an increased risk of suicidality. Additionally, the recent Braidwood case on preventive care access directly affects LGBT+ people in its treatment of Pre-Exposure Prophylaxis (PrEP). It relies, in part, on religious protections arguments to limit access to the drug based on the plaintiff’s claim that it “facilitate[s] and encourage[s] homosexual behavior, prostitution, sexual promiscuity, and intravenous drug use.” If PrEP use declines as a result of the Braidwood decision, HIV incidence could increase, likely disproportionally impacting people of color and LGBT+ people. Efforts to curtail access to gender affirming care and the Braidwood decision are at odds with the Administration’s stated approach to health equity for LGBT+ people. How such policies play out in the longer term will be determined largely by the courts.
Evolving immigration policies may impact the health and well-being of immigrant families. When the PHE ends on May 11, 2023, Title 42 restrictions that suspended the entry of individuals at the U.S. border to protect public health during the COVID-19 emergency are expected to terminate. It is anticipated that when the authority ends, there will be an increase in immigrant activity at the U.S. border. The Biden Administration has announced plans to increase security and enforcement at the border to reduce unlawful crossings, expand “legal pathways for orderly migration”, invest additional resources in the border region, and partner with Mexico to implement the aforementioned plans. However, it remains to be seen how shifting policies will impact trends at the border and health and health care in that region. The future of the Deferred Action for Childhood Arrivals (DACA) program remains uncertain, and its implementation is currently limited subject to court orders. If the DACA program is found to be unlawful in pending court rulings, individuals would lose their DACA status and subsequently their work authorizations. The loss of status and work authorization may result in loss of employer-based health coverage, leaving people uninsured and unable to qualify for Medicaid, CHIP, or to purchase coverage through the Marketplaces. Additionally, although the Biden Administration reversed public charge regulations implemented by the Trump Administration as part of an effort to address immigration-related fears that limited immigrant families’ participation in government assistance programs, including Medicaid and CHIP, many families continue to have fears and concerns about enrolling in these programs, contributing to ongoing gaps in coverage for immigrants and children of immigrants.
Growing mental health and substance use concerns and ongoing racism, discrimination, and violence may contribute to health disparities. As previously noted, mental health and substance use concerns have increased since the onset of the pandemic, with some groups particularly affected. These trends may lead to new and widening disparities. For example, people of color have experienced larger increases in drug overdose death rates than White people, resulting in the death rate for Black people newly surpassing that of White people by 2020. Further, Black and Asian people have reported negative mental health impacts due to heightened anti-Black and anti-Asian racism and violence in recent years. Research has documented the negative health impacts, including negative impacts on mental health and well-being, of exposure to violence, including police and violence. Research shows African American and AIAN men and women, and Latino men are at increased risk of being killed by police compared to their White peers. Black and Hispanic adults also are more likely than White adults to worry about gun violence according to 2023 KFF survey data. Other KFF analysis shows that firearm death rates increased sharply among Black and Hispanic youth during the pandemic driven primarily by gun assaults and suicide by firearm. Research further shows that repeated and chronic exposure to racism and discrimination is associated with negative physical and mental health outcomes, including premature aging and associated health risks, referred to as “weathering,” as well as higher mortality.
Despite growing mental health concerns, people of color continue to face disproportionate barriers to accessing mental health care. Research suggests that structural inequities may contribute to disparities in use of mental health care, including lack of health insurance coverage and financial and logistical barriers to accessing care, stemming from broader inequities in social and economic factors. Lack of a diverse mental health care workforce, the absence of culturally informed treatment options, and stereotypes and discrimination associated with poor mental health may also contribute to limited mental health treatment among people of color. Amid the pandemic, many states implemented telehealth behavioral health services to expand access to behavioral health care, and most states intend to keep these services. States are also adopting strategies to address workforce shortages in behavioral health. As states seek to expand access to behavioral health care, it will be important to ensure that services address the cultural and linguistic needs of diverse populations. Further, in 2022, the federal government mandated the suicide and crisis lifeline number that provides a single three-digit number (988) to access a network of over 200 local and state-funded crisis centers. The 988 number is expected to improve the delivery of mental health crisis care; however, it is unknown how well it will address the needs of people of color and other underserved populations.
Conclusion
In sum, disparities in health and health care for people of color and other underserved groups are longstanding challenges, many of which are driven by underlying structural and economic disparities rooted in racism. Addressing disparities is key not only from an equity standpoint but for improving the nation’s overall health and economic prosperity. Amid the COVID-19 pandemic, the federal government identified health equity as a priority and has since launched initiatives to address disparities wrought by the COVID-19 pandemic and more broadly. Alongside the federal government, states, local communities, private organizations, and providers have engaged in efforts to reduce health disparities. Moving forward, a broad range of efforts both within and beyond the health care system will be instrumental in reducing disparities and advancing equity.



