Millions will eliminate overall health insurance policy starting Saturday. But they could possibly not know it.
Tens of millions of folks will start out to shed their wellness insurance plan on Saturday, as 5 states start the unwinding of a pandemic-era defense that held men and women from being taken off from the Medicaid rosters.
Through the general public health crisis, states ended up expected to preserve individuals on Medicaid without having the often annually reapplication process commonly in place. But now that the general public health and fitness unexpected emergency is winding down, so are the Medicaid rolls.
“We’re now in a placement inside just a few of times where states can get started to disenroll people — to redo their rosters for Medicaid — and this ongoing protection necessity is no for a longer period likely to be in spot,” Dr. Avenel Joseph, vice president of policy for the Robert Wood Johnson Foundation, informed ABC News.
The difficulty that Joseph and other advocates are involved about is that not enough folks know they’re about to get kicked off their coverage.
For Jeffrey Jackson, a 62-yr-aged Medicaid beneficiary in Arkansas who faces dropping that coverage in a subject of times, that could be a “nightmare.”
Arkansas is a single of the 5 states that will begin getting rid of men and women from protection on April 1, together with Arizona, Idaho, South Dakota and New Hampshire.

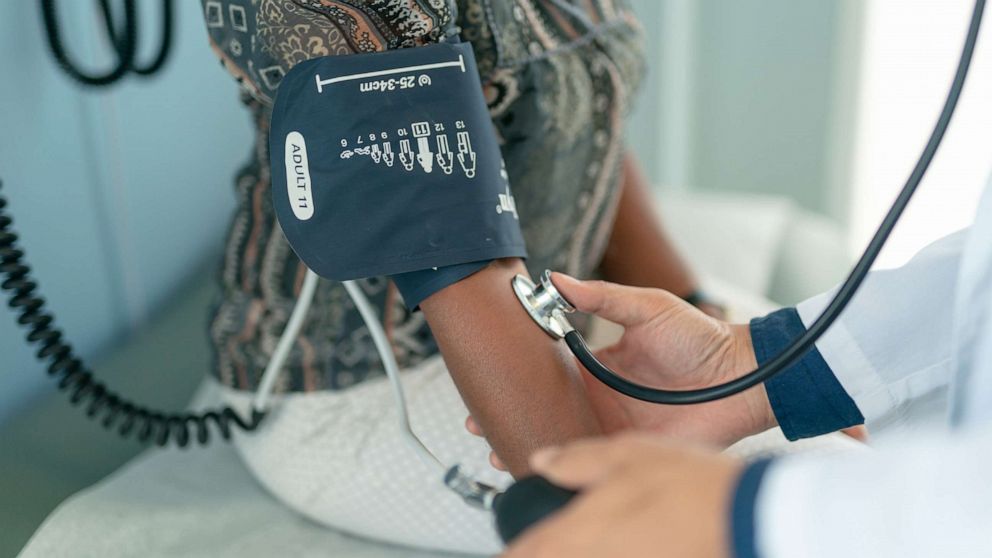
A girl sits on an examination desk in a clinic while a overall health care specialist checks her blood pressure.
Inventory Photograph/Getty Photos
Without having Medicaid, Jackson’s economical choices would have to appear down to “regardless of whether I would eat or no matter whether I will get my treatment.”
Jackson mentioned he’ll have to meet up with with his medical professionals to inquire them what drugs he can do devoid of.
“We are going to glance at what’s remaining and then I will say I will search at the selling price and what I can find the money for or are not able to pay for,” Jackson informed ABC Information.
Inspite of the dire stakes, getting rid of Medicaid is a common dilemma that utilized to happen annually just before the pandemic — the regular individual on Medicaid obtained about 10 months of protection a 12 months, because of something called “churn,” which often takes place when bureaucratic hurdles drive individuals out of the method for good reasons as very simple as missing a letter in the mail or relocating.
In accordance to estimates from KFF, a nonpartisan nonprofit that reports on nationwide well being challenges, about 65% of individuals who do get disenrolled close up uninsured for a portion of the pursuing year.
Obtaining back again on well being insurance can be challenging, Joseph stated.
“It can be not just like you examine a box and you can get back again on Medicaid the next working day. The approach of receiving re-enrolled in Medicaid, even when you might be qualified, can choose months. And throughout that interval of time, people — people today but also their families, and small children in certain — can fall through the cracks,” Joseph said.
The Section of Wellbeing and Human Services estimates that this time close to, just after a few years without having “churn” in the process, approximately 7 million Us residents who continue to qualify for Medicaid will drop rewards.
An additional 8 million will get rid of coverage since they no more time qualify and need to have outreach to fully grasp exactly where they can enroll in other, low-price tag federal government overall health programs as a result of the Reasonably priced Care Act, according to HHS.
“What we have heard from Medicaid directors throughout the states is this is the most significant shifting of insurance coverage protection for people considering that the Very affordable Care Act was set in position more than 10 several years ago,” Joseph said. “This is a significant endeavor.”
“And with that kind of motion,” Joseph reported, “susceptible folks will fall by way of the cracks.”



